Adhesive Remover
100% Organic Virgin Coconut Oil.
Invented by a NICU Nurse and Nurse Practitioner, Nurse Angele’s Wipes are designed to make the removal of medical adhesives easy and pain-free for patients, while also minimizing the risk of skin irritation and damage. May be used as massage and skin oil.
Order Wipes Parents Portal
For Use on All Types of Bandages & Dressings
Invented to be used on all adhesive dressings, such as hydrocolloids, transparent dressings, tapes, and bandages.
Natural & Organic
100% organic virgin coconut oil uses no toxic chemicals to break down adhesives.
Safe & Gentle on All Skin Types
For use on all patients from Neonates to Geriatrics. Gentle on fragile skin.
Anti-Viral
Anti-Bacterial
Anti-Fungal
Anti-Inflammatory
FDA Registered
Nurse Created & Approved
Key Uses for Nurse Angele’s Wipes.
Removes Adhesive Bandage & Dressings:
- EKG leads
- Hydrocolloids
- Silicone adhesive
- Tape and bandages
- Stoma wafers
- Wound and surgical dressings
Other Uses for Nurse Angele’s Wipes:
- Infant massage
- Reduces TEWL (Trans-Epidermal Water Loss) in premature infants
- May help with infant weight gain
- For use with breastfeeding mothers
Say Goodbye to Adhesive Injuries.
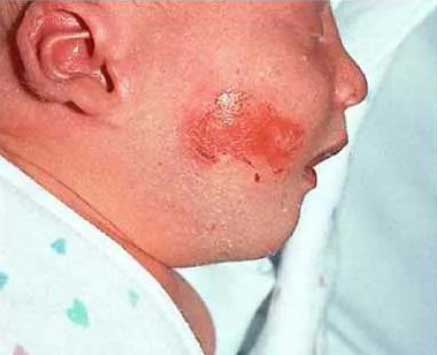
Adhesive injury is the most common source of skin breakdown in infants in the NICU. Particularly in premature skin, the layers of skin called the epidermis, outermost layer, and dermis, the next layer, are not as strongly bonded. Therefore, upon removal of adhesives, these layers are pulled apart and the epidermal layer is removed with the adhesive. This results in skin breakdown and increased risk of infection, pain, and if a large enough area is involved, fluid and temperature loss. Many studies discuss a decrease in skin barrier function which can also result in fluid or temperature loss without visible skin breakdown.
Nurse Angele’s Wipes
The gentle, organic, and non-toxic coconut oil is safe and effective, not only for adhesive removal, but also as a massage oil, moisturizer, and an aid to promote infant weight gain.
Epidermal Stripping.
Epidermal stripping, trans-epidermal water loss (TEWL), and irritation to sensitive skin from removing adhesives are among the reasons Nurse Angele’s Wipes were created. Neonates are at high risk for medical adhesive–related skin injuries (MARSIs). Gestational age is strongly linked to epidermal barrier function. The skin barrier of premature infants is injured easily and can serve as a portal of entry for agents, causing serious bacterial infections. Neonatal skin is 40%–60% thinner than the skin of an adult, with fewer epidermal cell layers. This leads to an undeveloped stratum corneum.
The decreased cohesion between the epidermis and dermis places the premature newborn at risk for skin injury when medical adhesives attached to the skin are removed. When adhesives are used, the bond between the adhesive and the epidermis may be stronger than that between the epidermis and dermis, resulting in stripping of the epidermal layer and decreased skin-barrier function. Removal of any of these layers of skin may lead to an increase in transepidermal water loss (TEWL) which may compromise fluid balance. It can also increase skin permeability and lead to toxicity from topically applied substances.
The risk of absorption and toxicity is greater in premature infants due to their immature Stratum Corneum skin barrier function. Preemies have a remarkably thinner epidermis and Stratum Corneum compared to full-term infants. The stratum corneum is 10–20 layers in both adults and full-term newborns. However, infant stratum corneum does not function as well as adult skin throughout the first year of life and is approximately 30% thinner than that of adult skin. Due to preterm infants’ impaired skin barrier function, they are at risk of unintended systemic absorption of topical substances. There is a confirmed high incidence of percutaneous toxicity from topical substances in premature infants.
Preemies and newborns are also at risk of percutaneous toxicity due to their large surface area to body weight ratio. A baby’s body surface is about three times greater than an adult’s, compared to the weight of his/her body.
Avoid using topical products that may be absorbed transdermally and cause toxicity. For example, toxicity can result from systemic absorption of alcohol from topical products.
Coconut Oil and Immunity: What do we really know about it so far?
Coconut oil as health oil was recognized in Ayurvedic medicine almost 4000 years ago. The same health effects were also attributed to the mother’s milk in ancient literature. Modern research has now found a common link between these two natural health products – their lipid content. The medium chain fatty acids and monoglycerides found primarily in coconut oil have miraculous healing power which act as natural antibiotic and also help modulate immunity. The information discussed in this review explains that coconut oil, either topically applied or ingested, gets broken down to release Lauric Acid and Monolaurin – known anti-microbial agents. The studies reported in literature are discussed to evaluate the antiviral, antibacterial and antifungal benefits of coconut oil.
Not only does coconut oil metabolites have antimicrobial activity but also these remarkable derivatives have been shown not to cause resistance organisms to appear. The anti-microbial mechanistic action also helps activate the anti-inflammatory nature of the immune response in human body.
In vitro, animal, and human studies support the potential of coconut oil as effective and safe immune-nutritive active. New and exciting health and industrial uses of coconut oil and its derivative are possible. Never before in recent times has the recognition of the positive health effects of coconut oil been stronger. And never before in the history of man is it so important to emphasize both need and efficacy of natural products known for their safety proposition. Immunity has been a buzzword in the current scenario and the demand for modulating immunity with natural means has been so unprecedented and so ubiquitous. Coconut oil and its value added forms can contribute to a more vigorous and healthy future.
Link to ArticleWhat Hospitals are Saying!
“We used to coconut oil wipes on our most recent micro preemie. This baby was born at 23.2 weeks. This baby only received 1 dose of antenatal steroids 6 hours before delivery. Over the course of this baby’s stay, they had a UAC for 7 days, a PIV for 10 days, and a PICC for 10 days. This baby also spent 41 days intubated on mechanical ventilation. This baby spent 93 days with us before being transferred at 36.4 corrected gestation for ROP eye treatment. This baby never had a positive blood culture (they had 3 blood cultures drawn is the first 20 days of their stay) and only had antibiotics for the first 10 days of life. We do believe that the coconut oil wipes played a vital part in that and helped with their skin integrity. We will now be using the wipes on our micro preemies”
“Nothing more satisfying than glistening your patient up in something that not only smells amazing but is so soothing to our little one’s sensitive skin. This product is a must have for any infant and it’s one we can’t do without in our NICU and Special Care Nursery. They really are so amazing. Everyone loves them!”
Test Results and Research Articles.
- Material Safety Data Sheet and Lab Reports Learn More
- Weight Gain and Infant Massage Learn More
- Sepsis Prevention Learn More
- CPAP Protocol Utilizing Nurse Angele's Wipes™ Learn More
- New Product Spotlight: Nurse Angele’s Wipes™ (neonatal INTENSIVE CARE Vol. 38 No. 1 Winter 2025) Learn More
- Effect of Tea Tree Oil and Coconut Oil on Nipple Crack Formation in the Early Postpartum Period Learn More
- Comparing the Efficacy of Breast Milk and Coconut Oil on Nipple Fissure and Breast Pain Intensity in Primiparous Mothers: A Single-Blind Clinical Trial Learn More
Directions for Use.
- Product solid at room temperature.
- If desired, use sterile or clean gloves.
- For porous adhesive dressings, first wipe the external surface generously.
- Next, gently pull up a corner of the dressing and then continually wipe the skin/adhesive interface while gently pulling off the dressing.
- If replacing a dressing, cleanse area with soap or shampoo to remove the coconut oil, rinse with water, then pat dry intact skin. (There is no need to remove excess coconut oil from skin unless dressing is to be replaced. You may massage directly on intact skin.)
- May use on hair.
Order Your Nurse Angele’s Wipes Samples Today.
Order SamplesEstablishment Information.
2211 South Telegraph Road No. 7230
Bloomfield Hills MI, US
jessica@warriornp.com